Diabetes
Diabetes mellitus is a disorder of insulin production or action which causes high sugar levels. It is divided into type 1 and type 2 diabetes. Type 2 diabetes is more common than type 1 diabetes and around 90 to 95 percent of people with diabetes have type 2 diabetes. There are several key differences between type 1 and type 2 diabetes.
The most important difference is in the hormone insulin. Insulin is a hormone made by the pancreas that allows your body to use sugar (glucose) from carbohydrates in the food that you eat for energy or to store glucose for future use. Insulin regulation helps keep your blood sugar level from getting too high (hyperglycemia) or too low (hypoglycemia).
People with type 1 diabetes do not produce enough insulin or any insulin at all. Insulin treatment is vital in this case.
People with type 2 diabetes still produce insulin; however, the problem lies with the cells in the muscles, liver, and fat tissues. They do not respond to the insulin effectively, thus making it difficult to regulate the sugar level.
As a result, the body tries to compensate by having the pancreas pump out more insulin. Eventually, over a prolonged period of time, the pancreas slowly loses the ability to produce enough insulin due to exhaustion, and as a result, insulin may then be required or the cells do not get the energy they need.
Southeast Endocrine Associates provides specialist medical care for people with diabetes. In particular, the focus is on optimising diabetes care, and screening for, and treating complications of diabetes. Doctors in the associates work closely with diabetes educators, dieticians, and podiatrists.
We aim to promote a team-based diabetes management by maintaining a close liaison with patients’ general practitioners.
We are also able to provide information on insulin pump therapy, including assessment of patient suitability and initiation of pump therapy. We aim to equip patients with the skills to make appropriate modifications in conjunction with their treating physicians/nurse educators.
Weight Management Service
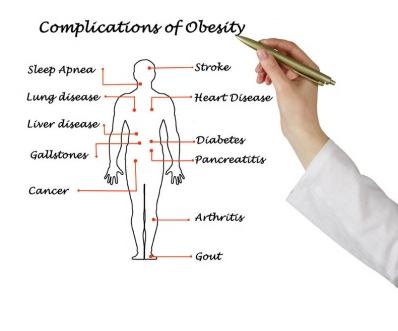
Obesity is fast becoming an epidemic throughout the world. It is a major risk factor for heart disease, cancers, arthritis and many other diseases. Patients with obesity are facing enormous difficulties in losing weight and this may cause significant anxiety and depression among patients.
Our endocrinologists can assist general practitioners in managing patients with obesity for weight management.
Problems identified by the patient and referring doctor will be addressed and the cause of weight gain identified where possible. Generally, a treatment regimen will be outlined in consultation with the patient’s wishes.
Our clinic management is based on current medical opinion on the practical management of obesity. Our specialists will try to improve the general health and well-being of patients through sustainable lifestyle changes, exercise and diet, and possibly medications.
We work closely with a number of bariatric surgeons and provide a multi-disciplinary approach to management of complicated weight management.
If you have a major weight problem, call us today to arrange for a consultation so we can assess a suitable treatment option for you.
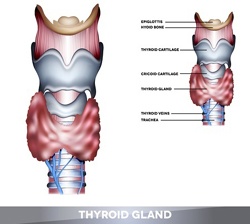
Thyroid Disorders
Thyroid disorders are common, and they include goiters (lumps), hyperthyroidism, and hypothyroidism.
About the thyroid
The thyroid is a small but important gland located superficially in the neck that produces and releases thyroid hormone called thyroxine.
The thyroid’s main role in the endocrine system is to regulate your metabolism, which is your body’s ability to break down food and convert it to energy. Food essentially fuels our bodies, and our bodies each “burn” that fuel at different rates. This is why you often hear about some people having “fast” metabolism and others having “slow” metabolism.
The thyroid keeps your metabolism under control through the action of thyroid hormone, which it makes by extracting iodine from the blood and incorporating it into thyroid hormones. Thyroid cells are unique in that they are highly specialized to absorb and use iodine. Every other cell depends on the thyroid to manage its metabolism.
Diseases and Disorders of the Thyroid
There are many diseases and disorders associated with the thyroid. They can develop at any age and can result from a variety of causes—injury, disease, or dietary deficiency, for instance.
But in most cases, they can be traced to the following problems:
- Too much or too little thyroid hormone (hyperthyroidism and hypothyroidism, respectively).
- Abnormal thyroid growth known as goiter
- Nodules or lumps within the thyroid
- Thyroid cancer
Southeast Endocrine Associates provides a comprehensive range of services covering the diagnosis, investigation, and management of the various thyroid disorders, including hypothyroidism, hyperthyroidism, thyroiditis, goitre, thyroid nodules, and thyroid cancers.
Osteoporosis
Osteoporosis—a condition marked by low bone mineral density, which leads to lowered bone strength and a heightened risk of fractures—is something you will not have to worry about until later in life.
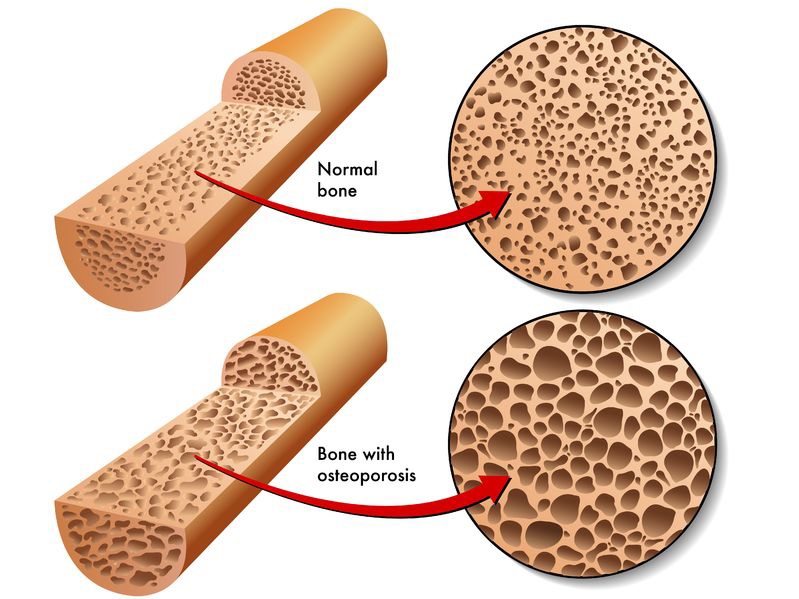
It is true—age is a leading risk factor for osteoporosis. Women over the age of 50 have the highest risk of developing the condition. Beginning in midlife, men and women begin to experience a decline in bone mass, with women losing bone quickly in the years following menopause.
However, people of all ages can develop osteoporosis, and age is just one of many risk factors for the condition. In fact, it is estimated that your genetic makeup accounts for 50-90% of your bone mass, while lifestyle and environmental account for the rest. That means that preventive lifestyle changes could reduce up to half of your osteoporosis risk.
That is why it is important to take early steps to improve your bone health. Additionally, if you already have osteoporosis or osteopenia (low bone mineral density that is not low enough to be considered osteoporosis), your specialist can help improve your bone health to protect against fractures.
Osteoporosis prevention requires a mix of eating right, appropriate physical activity, and active planning with your doctor to protect your bones.
It is never too early to begin taking care of your bones and working to prevent or delay osteoporosis.
Parathyroid Disorders and Hypercalcaemia
The parathyroid glands are four small glands located behind the thyroid gland that have the sole purpose of secreting parathyroid hormone to regulate our calcium level.
Calcium is an important element that helps the nervous and muscular systems function properly. A normal calcium level is required for optimal muscle contraction, and it is very important for the normal conduction of electrical currents in nerve cells.
The most common disorder of the parathyroid glands is hyperparathyroidism, which is characterized by excess parathyroid hormone (PTH), which causes high calcium levels. In other words, the parathyroid glands continue to make large amounts of PTH even when the calcium level is high, when they should not be making and releasing the hormone at all.
When one or more of the parathyroid glands are overactive, it releases too much PTH. This causes your bones to release calcium constantly into the blood stream. Without enough calcium in your bones, they lose their density and strength. Osteoporosis, characterized by this loss of calcium and bone density, is one of the common complications of hyperparathyroidism. Sometimes the calcium level can reach very high levels to cause other problems such as kidney stones, fractures and mental confusion. Surgery is the only potential curative therapy for this disorder.

Men’s Health
In men, testosterone is responsible for maintaining:
- sex drive
- sperm production
- facial, pubic, and body hair
- muscle
- bones
The amount of testosterone in a man’s body changes throughout the day, and it’s usually highest in the morning.
Low Testosterone Symptoms
If you have low testosterone levels, you may begin to notice the following signs and symptoms:
- decreased sex drive (libido)
- poor (or no) erections (erectile dysfunction or impotence)
- enlarged breasts
- loss of muscle bulk and strength
- weaker bones (osteoporosis)
- mood swings (including increased irritability, poor concentration)
- depression
In some men, low testosterone may be serious and they may experience more severe symptoms, especially the longer their testosterone levels remain low.
Low Testosterone
There are several causes of low testosterone level, and your doctor will work with you to figure out what’s causing your low levels.
Causes of low testosterone are divided into 2 main types: primary hypogonadism and secondary hypogonadism.
Primary hypogonadism is also known as primary testicular failure, and it is caused by a problem in the testicles. These problems can include:
- injury to the testicle
- Klinefelter syndrome
- undescended testicles:
Secondary hypogonadism is caused by a problem with the pituitary or hypothalamus glands. These glands produce hormonal signal to the testicles to make testosterone, thus if they are compromised, testosterone production can be affected.
Conditions that can cause secondary hypogonadism include:
- pituitary disorders
- medications
- type 2 diabetes and obesity
- aging
These are just some examples of what can cause male hypogonadism. Through the diagnostic process, our specialists should be able to figure out why you have low testosterone levels.
Women’s Health
Polycystic ovary syndrome
Polycystic ovary syndrome (PCOS) is a common condition affecting up to one in five women of reproductive age. Women might present with a variety of signs and symptoms, including irregular periods, unwanted hair growth, acne, and weight problems.
The symptoms of PCOS might vary in different individuals, and may include the following:
- Irregular periods—you may have your period less frequently than monthly (usually less than 8 per year), or not at all; you may also have the associated heavy bleeding
- Weight gain (yet some women with PCOS are thin)
- Excess hair growth on the male areas such as the face, chest, back, stomach, or upper arms and inner thighs
- Acne
- Oily skin
- Patches of thick velvety, dark skin (called acanthosis nigricans) on the neck, armpits, breasts, or thighs
- Thinning hair
- Difficulty getting pregnant
The treatment of polycystic ovary syndrome (PCOS) mainly focuses on managing the symptoms and prevention of metabolic consequences such as type 2 diabetes, obesity and heart disease. It is important to talk to us if you think you have PCOS symptoms as early treatment can help reduce your risk for long-term complications.
Menopause
Menopause is a normal part of aging. It refers to the time when ovarian reproductive function ends—when a woman’s ovaries stop producing eggs and making the hormones oestrogen and progesterone.
Menopause tends to occur in a woman’s late 40s to early 50s, but occasionally, women may have premature ovarian failure or early menopause. In addition, menopause may occur abruptly in a woman who has her ovaries removed or who undergoes chemotherapy or radiation.
Many women have difficulty with perimenopausal symptoms such as hot flashes, night sweats, mood changes, poor sleep, vaginal dryness etc. These can be managed with lifestyle changes and/or medications. It is also important to assess other health risks that occur with menopause. It is important to talk to us about these issues.
Diabetes and Endocrine Disorders in Pregnancy
What Is Gestational Diabetes?
Gestational diabetes sometimes develops when a woman is pregnant. It is when the blood glucose level (blood sugar level) of the mother goes too high during pregnancy.
If left untreated, elevated blood glucose level during pregnancy can be harmful to both you and your baby. Fortunately, our doctors are vigilant about checking for gestational diabetes so that it can be identified and effectively managed. Screening usually takes place at 24-28 weeks gestation or earlier in those at high risk. A pro-active treatment plan helps you have a good pregnancy and protects the health of your baby.
Treatment of gestational diabetes comes down to one main goal: controlling your blood glucose level so that it does not go too high. You can control your blood glucose level by eating well, exercising, and perhaps taking insulin or other medication. Not every woman with gestational diabetes needs medication or insulin.
You will know how well controlled your blood glucose levels are by monitoring it several times a day. Our doctors and diabetes educators will explain how to use a blood glucose meter, and when to check your levels.
You will also be asked to keep a record your daily levels—that helps both you and the doctor know how you are doing.
Thyroid Disease in Pregnancy
Thyroid diseases such as hyperthyroidism and hypothyroidism are relatively common in pregnancy and important to treat. The thyroid is an organ located in the front of your neck that releases hormones that regulate your metabolism (the way your body uses energy), heart and nervous system, weight, body temperature, and many other processes in the body.
If you have pre-existing thyroid conditions such as hyperthyroidism or hypothyroidism, you may require more medical attention to control these conditions during pregnancy, especially in the first trimester.
Diagnosis of Thyroid Disease in Pregnancy
Hyperthyroidism and hypothyroidism in pregnancy are diagnosed based on symptoms, physical exam, and blood tests to measure levels of thyroid-stimulating hormone (TSH) and thyroid hormones T4 and T3.
Treatment of Thyroid Disease in Pregnancy
For women who require treatment for hyperthyroidism, an anti-thyroid medication that interferes with the production of thyroid hormones is used. This medication is usually propylthiouracil (PTU) for the first trimester, and — if necessary, carbimazole can be used also, after the first trimester.
Hyperthyroidism may worsen in the first 3 months after birth, close monitoring is important, as our specialists may need to adjust the dose of medication.
Hypothyroidism is treated with a synthetic (man-made) hormone called levothyroxine, which is similar to the hormone T4 made by the thyroid. We will adjust the dose of your levothyroxine at diagnosis of pregnancy and will continue to monitor your thyroid function tests every 4-6 weeks during pregnancy.
Adrenal & Pituitary Disorders
Adrenal Disorders
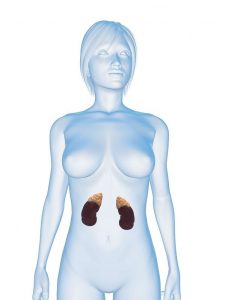 The adrenal glands are two glands that sit on top of your kidneys that are made up of two distinct parts.
The adrenal glands are two glands that sit on top of your kidneys that are made up of two distinct parts.
- The adrenal cortex—the outer part of the gland—produces hormones that are vital to life, such as cortisol (which helps regulate metabolism and helps your body respond to stress) and aldosterone (which helps regulate blood pressure).
- The adrenal medulla—the inner part of the gland—produces non-essential (that is, you do not need them to live) hormones, such as adrenaline (which helps your body react to stress).
Disorders and Diseases of the Adrenal Glands
There are multiple reasons why the adrenal glands might not work as they should. The problem could be with the adrenal glands themselves, or the root cause may be due to a defect in another gland that communicates with them such as the pituitary gland.
Below are the most common disorders and diseases of the adrenal glands:
- Primary aldosteronism – most common cause of secondary hypertension.
- Addison’s disease (Adrenal insufficiency)
- Cushing’s syndrome (Too much of “cortisol”)
- Congenital adrenal hyperplasia
The diagnosis and treatment of adrenal disorders can be quite complex and requires specialized care which may involve a multi-disciplinary team management. Your specialists at Southeast Endocrine Associates have the necessary team-based management approach to ensure the best care.
Pituitary Disorders
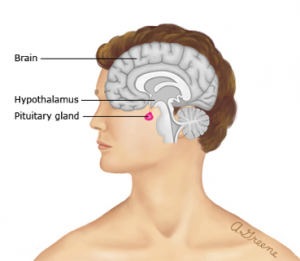 The pituitary gland (a.k.a the “master gland”) secretes hormones that control other parts of the endocrine system, namely the thyroid gland, adrenal glands, ovaries, and testes.
The pituitary gland (a.k.a the “master gland”) secretes hormones that control other parts of the endocrine system, namely the thyroid gland, adrenal glands, ovaries, and testes.
The pituitary gland is only about 1/3 of an inch in diameter (that’s about as large as a pea) and located at the base of the brain.
Pituitary tumours are the most common pituitary disorder, and many adults have them. However, they are not, in the great majority of cases, life threatening. But that does not mean that they are harmless—pituitary tumours can disrupt the gland’s normal ability to release hormones.
There are two types of pituitary tumours—secretory and non-secretory. Secretory tumors secrete too much of a particular hormone, and non-secretory tumours do not secrete hormone.
These hormonal imbalances can cause problems in many different areas of the body. If you have a secretory tumour that is overproducing prolactin hormone, for instance, you might experience unexplained milk secretion (galactorrhea) or irregular menses or infertility.
If you think you may have a problem with your pituitary gland, you should talk to our specialists. He or she will help diagnose and treat your hormone-related condition.
